November 7, 2023
Chronic obstructive pulmonary disease, or COPD for short, is a common, long-lasting lung disease. It is a progressive disease, which means its symptoms get worse over time.
There are several stages of COPD, each of which has different symptoms depending on how far the disease has progressed. Here’s more about the stages and how to contact Healthcare Associates of Texas if you need help managing this condition.
What Is COPD?
 COPD is a lung disease that makes it difficult for you to breathe. In COPD, less air flows in and out of the airways to cause breathing problems.
COPD is a lung disease that makes it difficult for you to breathe. In COPD, less air flows in and out of the airways to cause breathing problems.
There are two types of COPD: emphysema and chronic bronchitis. If you have COPD, you likely suffer from both types.
Emphysema occurs when the walls between the air sacs in the lungs become damaged. Normally, these air sacs will stretch easily when you breathe, but damage to them can prevent them from filling and deflating as easily.
Chronic bronchitis occurs when the lining of the airways becomes irritated and inflamed. This can cause thick mucus to form in the airways, which makes it hard for you to breathe.
At this time, there is no cure for COPD. However, it can often be effectively managed when detected and treated early on.
How Many Stages of COPD Are There?
There are four stages, or grades, of COPD. Dividing this disease into different stages makes it easier for doctors around the world to diagnose and treat.
Stage 1 COPD is the least severe, while stage 4 is the most severe. Stage 4 of COPD is also sometimes referred to as end-stage COPD.
What Are the 4 Stages of COPD?
Symptoms and treatments for COPD will vary based on the stage you are diagnosed with. COPD is usually diagnosed using a tool called a spirometer.
A spirometer can measure the force and speed at which you exhale. When you are given the spirometer test, your doctor will grade your results from grades 1 to 4, correlating with the four COPD stages.
Stage 1: Early COPD
This stage is the mildest form of COPD. With stage 1, you may not have any symptoms, and you may not know there is a problem with your lungs. Any symptoms you do have may resemble those of the flu, such as cough and mucus production.
Stage 2: Mild COPD
Symptoms of stage 2 COPD are usually worse and more noticeable than those of stage 1. Most people with this stage of mild COPD will visit their doctors for a checkup and diagnosis. In addition to having more severe coughing and mucus production, you may also experience shortness of breath when doing mild activities like walking.
Stage 3: Severe COPD
Stage 3 COPD is severe. In many cases with stage 3, breathing becomes difficult to the point you may not be able to leave your home. You may also feel extremely tired all the time.
In addition to experiencing severe coughing and shortness of breath during stage 3, you may also experience wheezing, tightness in the chest, swelling in the ankles, and frequent illnesses.
Stage 4: Very Severe (End-Stage) COPD
Stage 4 is the worst and most severe stage of COPD. During this stage, your blood oxygen levels are low enough to put you at risk for lung or heart failure. You will also experience difficulty breathing even when relaxing and resting.
The symptoms and flare-ups you may have with end-stage COPD can reduce your quality of life and may even be fatal.
Risk Factors for COPD
Smoking is the number one cause and risk factor of COPD. Up to 75% of people who have COPD are current or former smokers.
The chemicals and toxins in cigarette smoke can damage the airways and air sacs in the lungs to cause COPD. If you smoke, quitting right away may significantly reduce your risk.
Other risk factors of COPD include:
- Exposure to lung irritants. Air pollution, secondhand smoke, and chemical fumes may contribute to COPD.
- Age. COPD is more common in people aged 40 and older.
- Infections. HIV and tuberculosis are conditions that may increase your risk for COPD.
- Alpha-1 antitrypsin (AAT) deficiency. This genetic condition increases your risk.
- Asthma. One in five people with COPD also have asthma.
The Importance of Getting Tested for COPD
If you think you have COPD, getting tested for it can lead to early diagnosis and treatment. Early treatment of COPD may prevent your disease from getting worse.
COPD can be diagnosed with a review of your personal and family medical history and with spirometry.
Spirometry can determine whether you have COPD even if you don’t have symptoms. During this test, you will be asked to take a deep breath and then blow as hard as you can into a tube. The tube is connected to a machine called a spirometer.
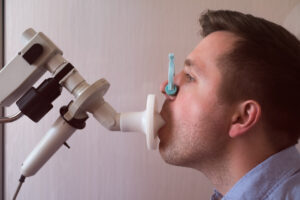
Next, you will be asked to inhale a medicine that opens your airways before blowing into the tube again. Your test results will reveal whether you have COPD.
Your doctor may also have you
do other lung tests to properly diagnose COPD. These tests may include:
- Peak expiratory flow (PEF) test. This test measures how fast you can blow air out of your lungs.
- Fractional exhaled nitric oxide (FeNO) test. This test measures the amount of nitric oxide in your breath and can reveal whether you have inflammation in your lungs.
- Arterial blood gas test. This test measures levels of oxygen and carbon dioxide in your blood.
- Chest computed tomography (CT) scan. A CT scan takes pictures of the insides of your chest and lungs.
- Chest X-ray. This is another test that displays images of the insides of your chest.
Tips for Living With COPD
COPD cannot be cured, but certain lifestyle practices and behaviors may slow its progression and reduce your symptoms.
Here are tips for managing COPD:
- Don’t smoke. Smoking can worsen your COPD and make it progress more quickly. Stop smoking and ask your doctor about smoking cessation treatments if you need help quitting.
- Eat highly nutritious foods. Breathing problems can often interfere with your appetite and the way you eat. Your doctor may recommend eating small amounts of highly nutritious foods to prevent nutritional deficiencies. Fruits, vegetables, and fish are examples of healthy foods you may need to eat.
- Avoid foods that cause bloating. Bloating may worsen your breathing problems. Your doctor may suggest avoiding any food that causes bloating. Beans, broccoli, cauliflower, beer, and fried foods are some of the many foods you may need to avoid.
- Wear loose-fitting clothes. Comfortable and loose-fitting clothes can make it easier for you to breathe and move around.
- Avoid lung irritants. Secondhand smoke, gas fumes, and cleaning products are examples of irritants that can worsen your symptoms.
- Exercise regularly. Exercise can increase your lung capacity and strengthen your lung muscles. Do mild activities at first, and gradually work your way to a higher intensity level.
Contact your doctor right away if you think your COPD is getting worse. Your doctor can work closely with you to find the right treatments that can make you feel better and slow the progression of your disease.
Request an appointment with Healthcare Associates of Texas today to receive treatment for any medical condition, including COPD. We offer a variety of primary care services, including wellness exams, screenings, and more.
References
- “What Is COPD? | NHLBI, NIH.” 2022. NHLBI, NIH. March 24, 2022. https://www.nhlbi.nih.gov/health/copd.
- “Causes and Risk Factors | NHLBI, NIH.” 2022. NHLBI, NIH. March 24, 2022. https://www.nhlbi.nih.gov/health/copd/causes.
- National Library of Medicine. n.d. “COPD.” Chronic Obstructive Pulmonary Disease | MedlinePlus. https://medlineplus.gov/copd.html.
- “Diagnosis | NHLBI, NIH.” 2022. NHLBI, NIH. March 24, 2022. https://www.nhlbi.nih.gov/health/copd/diagnosis.
DISCLAIMER
The information featured in this site is general in nature. The site provides health information designed to complement your personal health management. It does not provide medical advice or health services and is not meant to replace professional advice or imply coverage of specific clinical services or products. The inclusion of links to other web sites does not imply any endorsement of the material on such websites.