February 25, 2021
Diabetes is a serious disease that affects your whole body in many different ways. When your blood sugar levels are too high, your blood vessels can’t function properly and there are a number of complications that can arise. One complication is diabetic retinopathy, which is a disease of your retina and optic nerve.
Your eyes are important to you. Vision loss and eye problems can have serious implications on your life. Retinopathy is a scary disease that can start out with zero symptoms but eventually cause blindness. As you are dealing with diabetes complications, be sure you are consulting your doctor about diabetic retinopathy to help guarantee your eyesight is checked periodically and in case of problems, treated accordingly.
What is retinopathy?
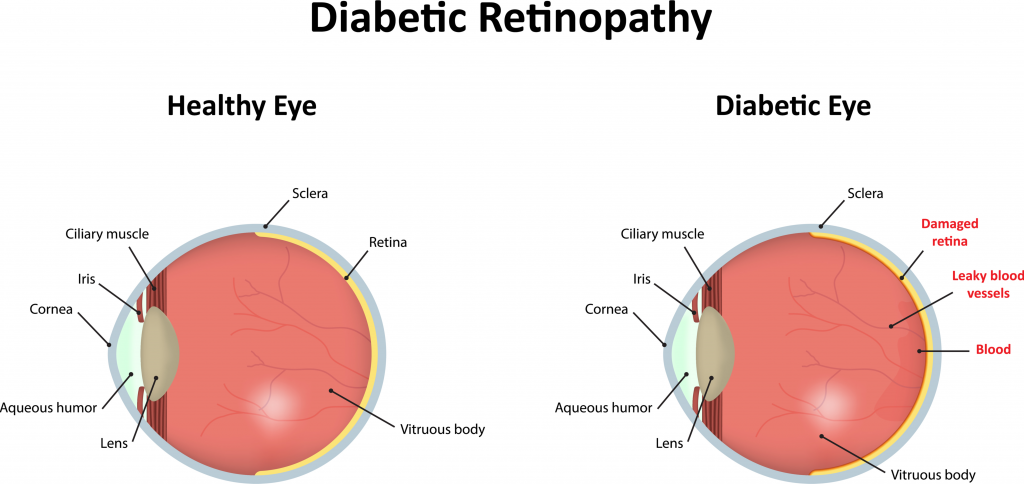
As always, it is important to understand your disorder as you start to ask questions about your health and medicine. So what is diabetic retinopathy? Simply put, it is an eye condition that affects the blood vessels in your retina in the back of your eye. Depending on how advanced the disease is, this can cause symptoms of blurred vision, spots in your eyesight, vision loss, or even complete blindness. Early cases usually cause zero symptoms, but can still be detected with periodic eye exams. Stay on top of your retinopathy with regular eye exams to help avoid vision problems down the line. There are two distinct stages of retinopathy that you may encounter: Non-proliferative diabetic retinopathy and proliferative diabetic retinopathy.
NonProliferative Retinopathy
Nonproliferative retinopathy is an early stage of this diabetic eye disease. Many individuals with diabetes may have this without even realizing it. In this stage, the blood vessels in your retina may start to leak or swell. Your macula is the part of the eye that helps you perceive things and when this begins to swell, it can cause vision loss. Over time, nonproliferative diabetic retinopathy can become severe, block off blood vessels, and cause problems for your central vision.
Proliferative Retinopathy
A more advanced stage of diabetic retinopathy is known as proliferative retinopathy. This is when your regular blood vessels are completely cut off and the eye begins growing abnormal blood vessels as a replacement. This neovascularization will bleed or leak a jelly-like substance into your vitreous which can cause dark floaters in your vision or a loss of vision altogether.
Risk Factors
The leading cause of retinopathy is diabetes, but there are other risk factors that may affect your eye health. For example, individuals with high blood pressure or high cholesterol should also be on the lookout for signs and symptoms of retinal complications. If you are a diabetes patient, your risk increases when you are pregnant or if you are addicted to tobacco. While these factors increase your risk, anyone with type 1 or type 2 diabetes has a risk of diabetic retinopathy.
Complications
Diabetic retinopathy can lead to many complications such as retinal hemorrhages or bleeds, glaucoma, and retinal detachment. A hemorrhage is bleeding into your vitreous and can cause temporary or permanent vision loss depending on the severity. You may also experience glaucoma. This is a pressure in your eye that can damage the nerves that communicate what you are seeing to your brain. Lastly, retinal detachment is a severe side effect of diabetic retinopathy. This is when the scar tissue formed from abnormal new blood vessels causes your retina to detach from the back of the eye. All of these complications can eventually lead to blindness.
When to see a doctor.
If you are at high-risk for retinopathy because of diabetes, you should already be consulting your doctor about your blood glucose levels on a regular basis. As part of diabetes management, you also should have retinal scans at least once a year with your primary care physician or the ophthalmologist. However, it may be time to consult a specialist or optometrist at any time if you are noticing irregularities or vision changes. You will need a comprehensive eye exam if you are noticing spots or floaters in your vision field, blurry vision, double vision, eye pressure, or trouble seeing your peripherals. Prevention and diabetes management are the first step to take toward avoiding complications, but if symptoms persist, it’s time to consult a doctor.
Getting a Diagnosis
There are a few different ways experts will diagnose retinopathy. Since the blood vessels of the retina are so small, you need a diabetic eye exam to detect early stages and signs of diabetic retinopathy. This will usually involve dilated eye exam. Your optometrist or ophthalmologist will use special eye drops as the best way to view veins at the center of the eye. This allows them to search part of the retina for abnormal blood vessels, swelling, growth of scar tissue, bleeding, retinal detachment, and other optic nerve irregularities.
Other potential tests may include a fluorescein angiography where an injection of dye into your veins travels to your eye to show any blockage or leaks. Your doctor may also try optical coherence tomography. This involves scanning your retina to gauge the thickness and see if any swelling has occurred. Your eye doctor can also run more standard tests of your vision and eye pressure to see if you may also have cataracts or glaucoma. With different ways to assess your eye health, early detection is possible. This is key to prevent complications in the later stages of retinopathy.
Treatment Options
Depending on your diagnosis of retinopathy, there are different options for treatment. If you are in the early stages of diabetic retinopathy, you may not need to do anything except monitor the situation with your eye doctor. Prioritize lowering your high blood glucose and managing your insulin and diabetes medical condition.
Early treatment may involve medication to help lower the macula swelling such as steroid shots directly into the eye. Steroid shots can help reduce swelling and even stop the growth of abnormal blood vessels within your retina.
Laser surgery is another treatment to help diabetic retinopathy. Photocoagulation is a procedure that burns the ends of the abnormal blood vessels to stop them from leaking fluids into the vitreous. Another option is panretinal photocoagulation – this is a procedure that can actually shrink these abnormal blood vessels so that they will not affect your eye or cause serious vision problems. These treatments usually involve a few sessions of laser therapy depending on the progression of the disease.
When the diabetic retinopathy progresses to become a medical emergency, surgery may be the only way to prevent total blindness. In addition to laser surgery, a vitrectomy may also be considered. This is when a tiny incision is made in the eye to release some of the fluid and blood from the retina to restore regular, healthy vision. This procedure usually involves a longer recovery period.
Prevention
Diabetic retinopathy is a difficult illness, since permanent damage may cause blindness. The best way to prevent these devastating long-term effects is through good diabetes management and regular screening for retinopathy. Continue checking your A1C and watching your overall health. Periodic exams with your primary care physician will go a long way to give you peace of mind that you are taking care of your body in the most effective way. Vision loss secondary to diabetes is a hard thing to live with, and is preventable and treatable. So please take your medications as prescribed, follow the dietary and exercise advice of your doctor, follow up regularly with your primary care physician, and do the eye exam periodically as advised.
DISCLAIMER
The information featured in this site is general in nature. The site provides health information designed to complement your personal health management. It does not provide medical advice or health services and is not meant to replace professional advice or imply coverage of specific clinical services or products. The inclusion of links to other web sites does not imply any endorsement of the material on such websites.
